While many of us have come to associate “orthotics” with corrective shoe inserts, the term actually refers to any external device used to adjust the function of the neuromuscular or skeletal system. These devices can be rigid or soft and include splints, braces, and wraps.
Pediatric orthotics is the use of these devices to immobilize, protect, or correct the position of a child’s bone.
According to Great Basin Orthopaedics (GBO) occupational therapist Chelsea Gonzalez, OTD, OTR/L, orthotics can be used on the very youngest of children. “Even preemies in the NICU can benefit from orthotics,” says Gonzalez. “The materials are a bit different than what we’d use for a five-year-old, but the goal is the same — to stabilize and correct positioning.”
Common uses for pediatric orthotics
Pediatric orthotics can support, protect or immobilize joints for healing; restrict unwanted motion; correct existing deformity; restore mobility; or serve as a basis of attachment of specialized devices to assist with function. They can be used to heal injury and correct congenital or neuromuscular conditions, including the following:
Injuries
- Brachial plexus birth palsy
- Fracture
- Ligament/tendon injury
- Nerve injury
- Burns
Congenital conditions
- Camptodactyly
- Clinodactyly
- Syndactyly
- Hypoplastic thumb
- Indwelling thumb
- Trigger thumb
Neuromuscular conditions
- Cerebral palsy
- Rheumatic conditions
The conditions that Gonzalez — a fellowship-trained pediatric hand therapist — commonly treats with pediatric orthotics at the GBO clinic include upper extremity fractures, fingertip crush injuries, nerve injuries, cerebral palsy, indwelling thumb, neurofibromatosis, burns, congenital trigger thumbs, tendon lacerations, and soft tissue strains.
The difference between orthotics and casts

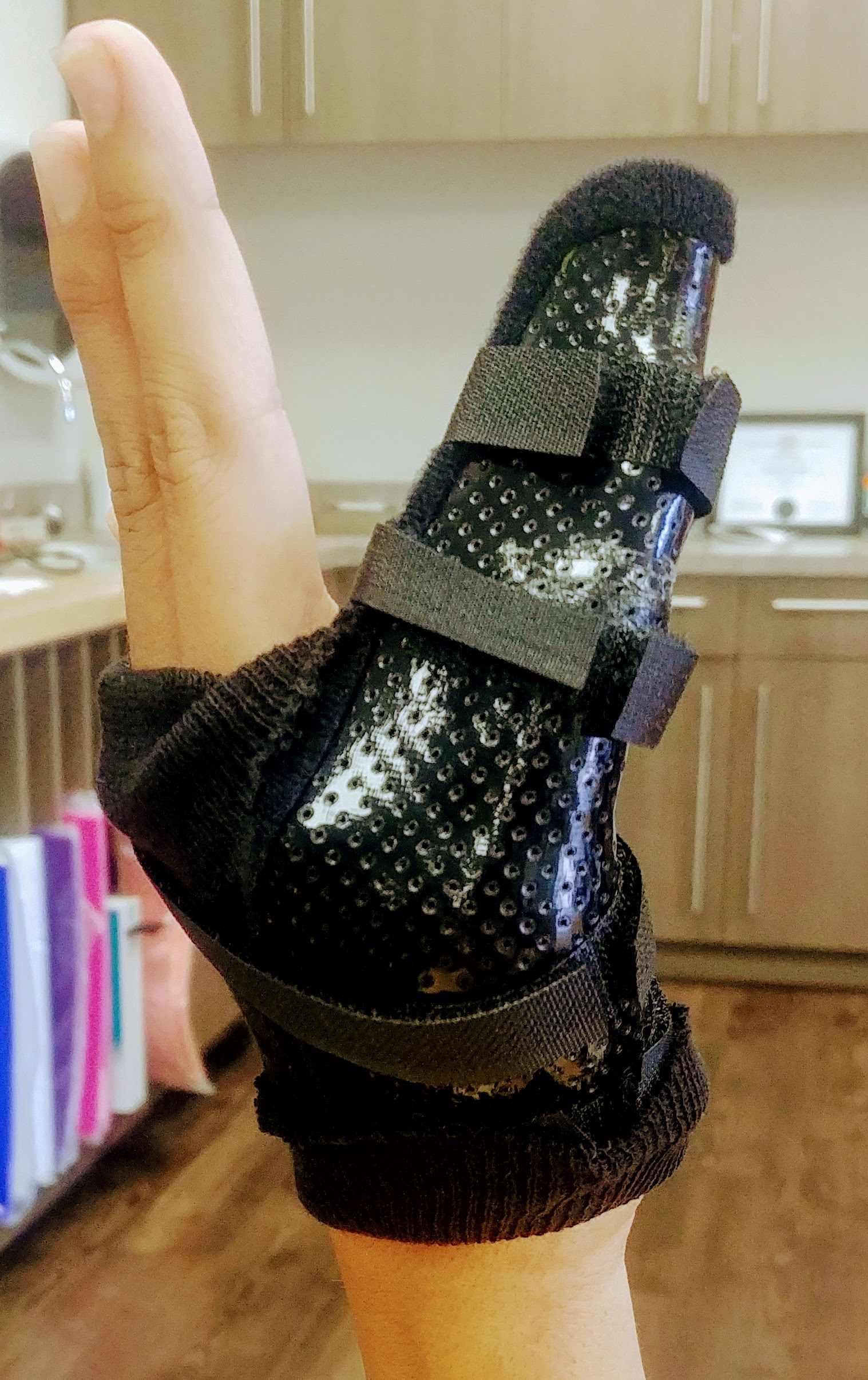
While they serve similar functions, orthotics and casts are different. Orthotics can be taken on and off for bathing and movement therapy. Straps on the orthotic allow for easy adjustment and sizing changes as healing progresses or swelling decreases. Orthotics are made with materials such as Thermoplast (a moldable plastic), metal rivets, Velcro strapping, neoprene, padding, and microfiber lining or lacing.
Casting is used when an orthopaedist prescribes complete immobilization. Casts provide rigidity and enhanced support to allow undisrupted healing and are highly beneficial for complex bone fractures or ligaments that would be disrupted by early active motion. A cast cannot be taken on and off and must be removed using a special saw at the end of treatment. Casts in the U.S. are typically made of fiberglass.
The nature of injury, and sometimes the age or tolerance of the patient, will dictate which corrective tool is used.
Orthotics are custom made for each patient
Like casts, customized orthotics are designed for a specific patient and can only be worn by them. Occupational therapists like Gonzalez are trained in the fabrication of customized orthotic supports. In collaboration with GBO physicians, she analyzes the level of injury, patient information and desired healing outcomes to design a support that will best serve the patient’s needs.
Kids aren’t just little adults
While orthotics are used to heal adults and kids, kids require some special adjustments. During her fellowship training, Gonzalez learned about the unique needs of pediatric patients and how to effectively address them.
Among those needs is keeping the orthotic in place. Children, especially the very young, may be oblivious to the needs of their healing joint and not adjust their activity accordingly. Pediatric orthotics need to be quite sturdy, yet flexible for active kids. A typical Velcro enclosure may not work for a young child accustomed to removing shoes with Velcro, and laces with a double knot may be needed to keep it secure. The flexibility of an orthotic can also adjust for growth if the device is required long term.
Gonzalez has also learned that it pays to play a little when it comes to pediatric orthotics. “We’ve used tie-dyed shoelaces, stickers, glitter pens,” she explains. “It makes it personal for the kids. And if they like their orthotic, they’re not as likely to try and remove it.”
Seeking an evaluation
Most parents will be referred to a pediatric hand therapist like Gonzalez by their orthopaedist or a primary care physician. However, there are times when they may seek assessment of a condition on their own. If you are a parent and have any concerns related to your child’s hand use – ability to write, hand strength, or fine motor skills — contact GBO for expert evaluation at 775.786.1600.